Lung Ultrasound Theory & Principles
Lung Ultrasound Theory & Principles
Unlike cardiac and abdominal ultrasound, lung ultrasound is unique in that the majority of its interpretation is based on artifact and not real anatomy. The lung is predominantly composed of air, which is a poor transmitter of ultrasound waves. In a normal aerated lung, the ultrasound waves scatter below the pleura.
Recall: in contrast to fluids, gas scatters ultrasound waves
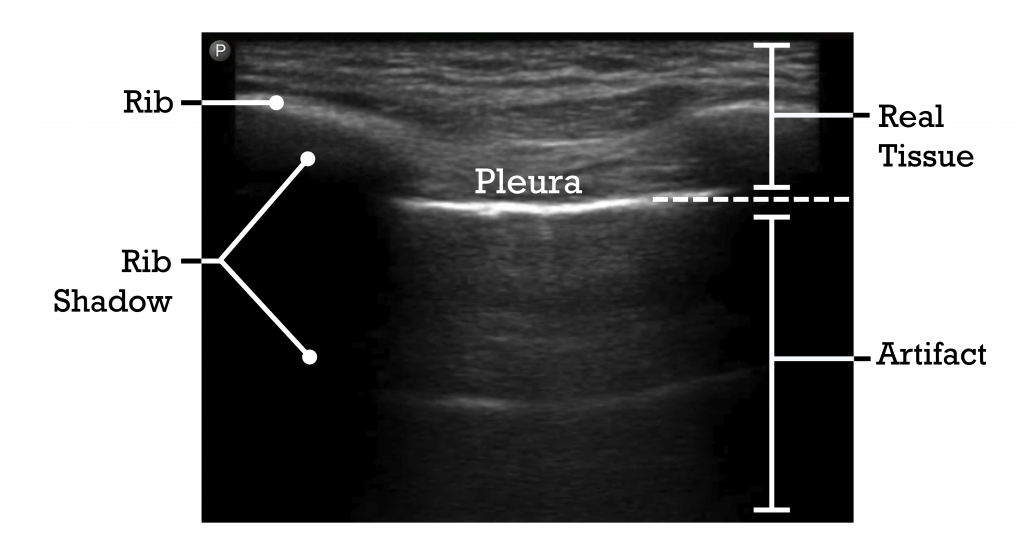
The pleural line is the first horizontal hyperechoic horizontal line that is immediately deep to the ribs. The pleura is comprised of parietal and visceral pleura, which in the normal lungs are in contact with each other creating a single hyperechoic line. These two pleura create a potential space, and in the setting of a pleural effusion become separated, with the parietal pleura lining the chest cavity and the pleura lining the lungs. On a lung ultrasound image, the area superficial to the pleura is real anatomy, such as soft tissue, muscle, and ribs. In contrast, the image deep to the pleura is generated by artifact and, thus, is not real anatomy. This includes rib shadows (as ultrasound waves cannot penetrate through bone) and artifacts such as A-lines and B-lines (discussed later).
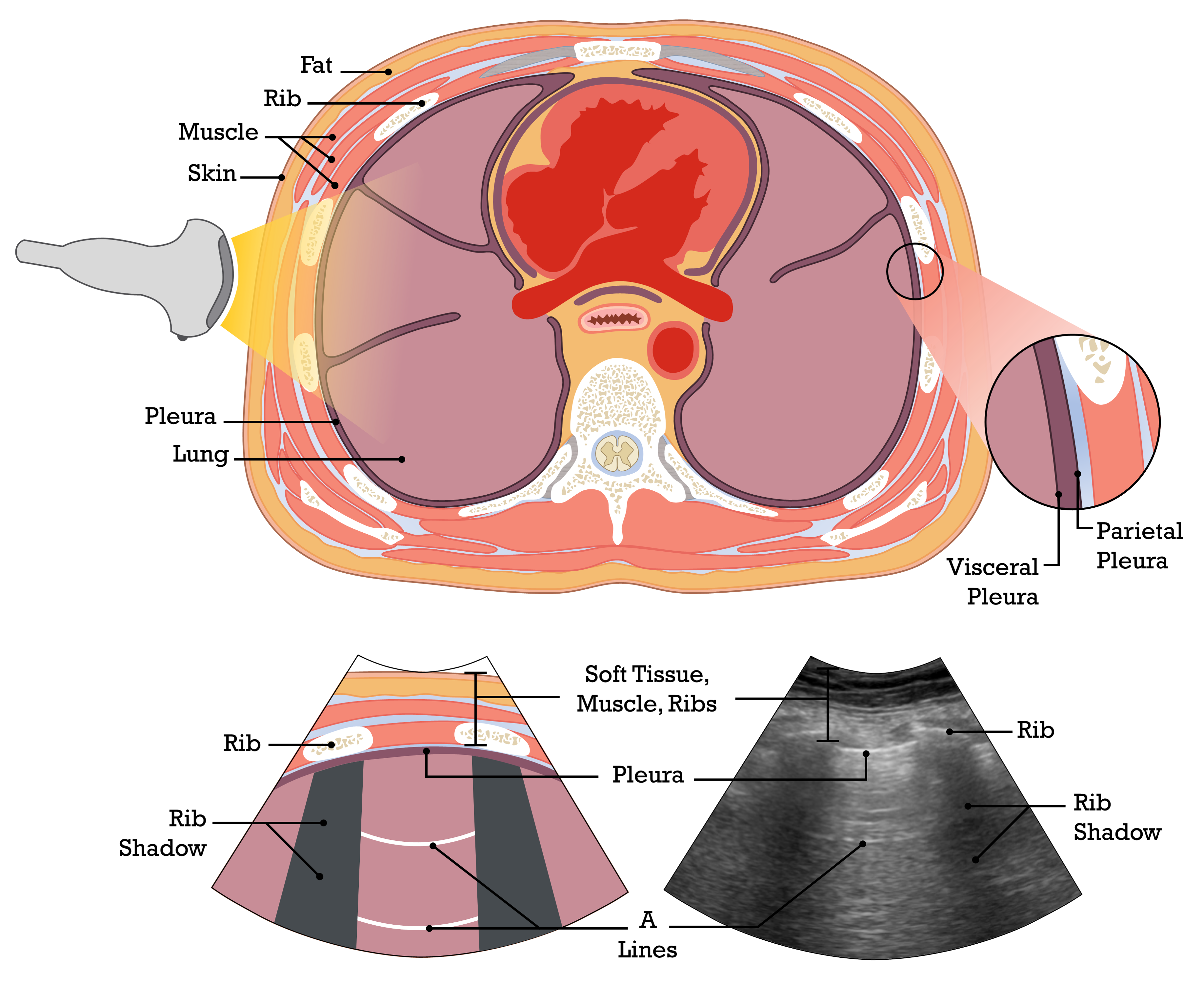
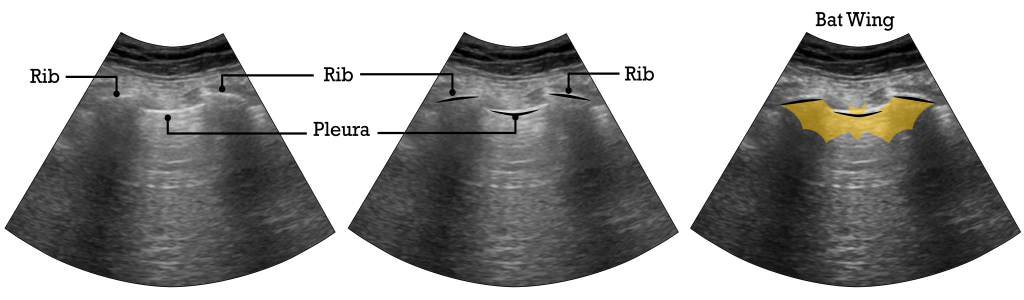
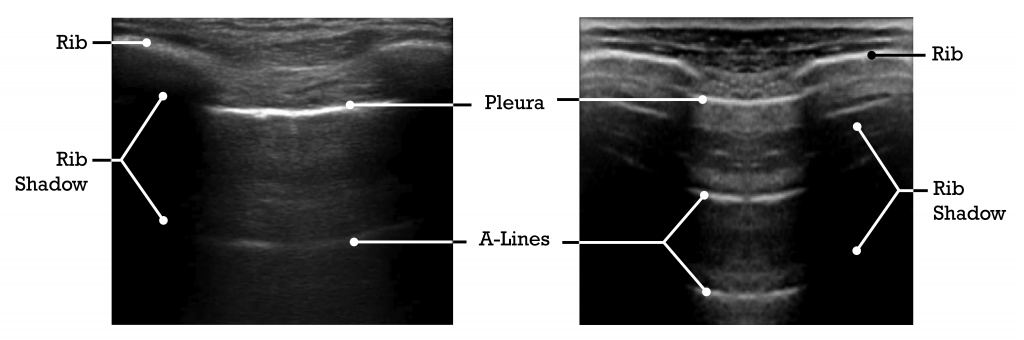
Normal Ribs and Pleura: Bat Wings
Note the three horizontal hyperechoic lines created by the ribs and the pleura when an ultrasound probe is placed between the ribs. These three lines create an image similar to a ‘Bat Wing.’ This can be used to help identify the major landmarks of a lung ultrasound.
A-Lines & B-Lines
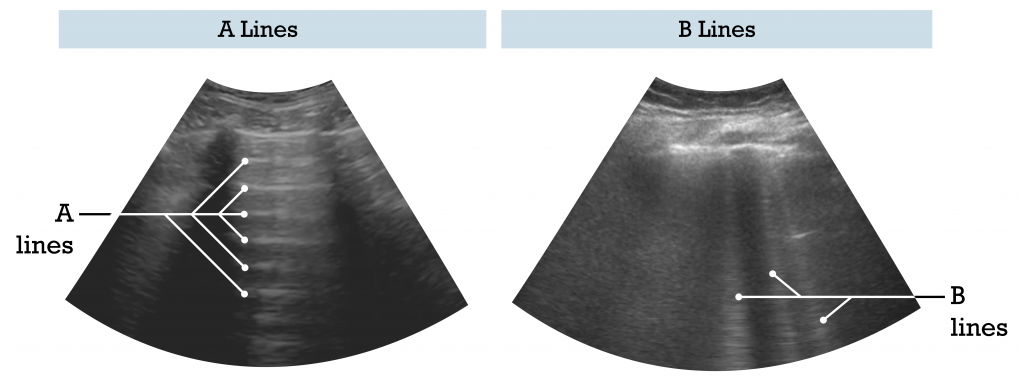
A-Lines
A-lines are reverberation artifacts and appear similar to the pleural line; they are evenly spaced horizontal lines deep to the pleura. An A-line occurs when the ultrasound beam is reflected back and forth between the probe and the pleura. This produces a similar line that is equidistant from the top of the screen to the pleural line. The presence of A-lines indicate that region of the lung is properly aerated.
A-lines are artifacts that appear as evenly spaced horizontal lines below the pleura caused by the ultrasound beam being reflected back and forth between the probe and pleura.
B-Lines
When any non-air substance is present in the lung, it will generate artifacts known as B-lines. A B-line is an artefact that appears as a vertical, pleural based hyperechoic line that moves with respiration. They extend to the end of the screen and are at least 18cm in length. They must also obliterate A-lines if they intersect them.
B-lines are vertical lines that appear when a non-air substance is present in the lung, such as fluid.
Healthy lungs may have B-lines; however, the presence of 3 or more B-lines within a single intercostal space is considered pathological. Pathological B-lines indicate an interstitial syndrome is present. Interstitial syndrome itself has its own differential including: pulmonary edema, diffuse alveolar hemorrhage, pneumonitis, ARDS and pulmonary fibrosis. Anything that increases the density of the lungs, will create B-lines (the same differential as any process that creates an opacity on a Chest X-Ray).
Due to a high baseline prevalence, B-lines are commonly associated with pulmonary edema from congestive heart failure. In this case, B-lines are produced by fluid filling the intralobular septum, akin to Kerley B-lines on chest X-ray. However, be careful – 3+ B-lines does not always mean heart failure. Remember that interstitial syndrome has its own differential diagnosis as listed above.
Watch the following video demonstrating B-lines.
A-lines and B-lines are mutually exclusive. A-lines are caused by a reflective air-filled lung, while B-lines are created by ultrasound waves penetrating into the lung parenchyma (or at least intralobular septums).
Additional Resources
For more information about the basics of lung ultrasound and B-lines, watch this video.
